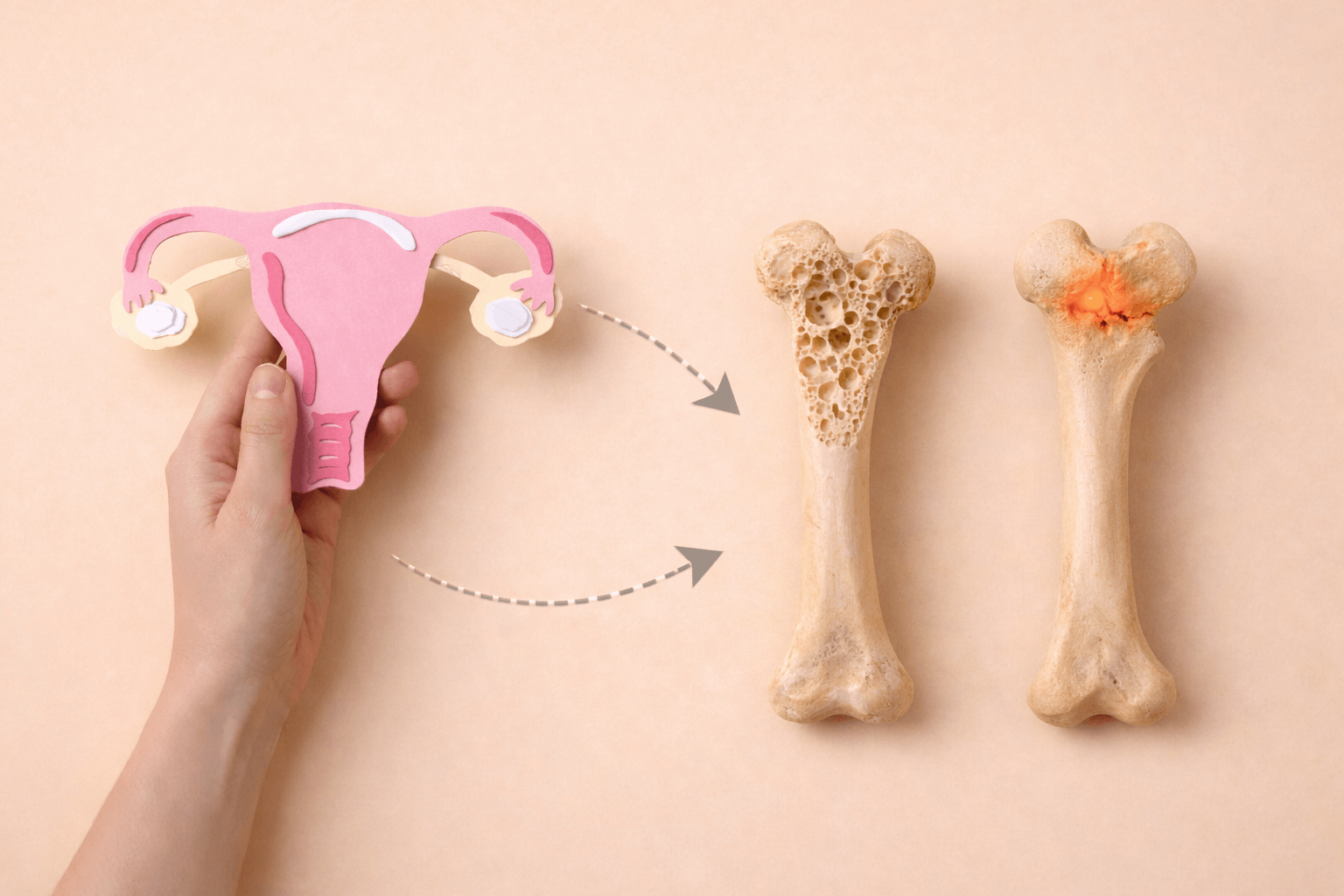
Menopause is a significant turning point in a women’s life and is often associated with changes like irregular periods, hot flashes, night sweats, mood change which may affect the quality life1. What’s less visible, but equally important, is what’s happening inside the body, particularly to bones.
Bone loss during menopause transition and post-menopause is often silent, gradual, and may remain unnoticed until a fracture occurs2. Understanding this connection early may help women make informed decisions about nutrition, lifestyle, physical exercise and consider dietary supplements that support skeletal strength, if required.
Bone loss prevention is an important concern in menopause journey and during the menopausal stage.
What Happens to Bones During Menopause transition period?
Bones are living tissue that constantly undergo process of breaks down and renewal. Till the time of peak bone mass this process stays balanced but with increasing age your body begins to lose bone faster than it can be replaced3. Scientific studies have shown that women tend to show faster bone loss than men4,5.
Estrogen is a female hormone, which plays a protective role in bones by slowing bone breakdown. However, with increasing age (40-55 years) estrogen levels may start to decline resulting in accelerated bone resorption than bone formation leading to a net loss of bone density causing fragile bones.6
Research suggests that there may be rapid, often exceeding 2% annually bone loss in first 5 years of menopausal transition period7 and may even lose up to 20% of their bone mass during menopause phases.2. This accelerated phase of bone loss may primarily be driven by low levels of estrogen in the body along with other contributing factors.2
Why Bone Loss Accelerates During Menopause
The years around menopause, peri-menopause and post-menopause are critical for bone calcium preservation. Several factors come into play:8
- Faster bone turnover due to low estrogen
- Reduced calcium absorption efficiency with age
- Lower Vitamin D synthesis due to less sunlight exposure
- Decreased physical activity in later years
Together, these changes may affect the bone strength and may further increase the risk of osteopenia (low bone mass) or even osteoporosis, a condition in which bones become weak and are more likely to break, over time.
The Role of Calcium and Vitamin D3
It is well-known fact that adequate dietary calcium intake is essential for bone strength. During menopause apart from estrogen depletion, the body’s ability to retain calcium may also become less efficient9.Thus, adequate calcium and vitamin D intake from diet or through nutritional supplement, if required, may help to support the calcium requirement of the body.
Calcium and Vitamin D3 work together to support bone mineralisation:
- Calcium provides structural strength
- Vitamin D3 improves calcium absorption and supports bone remodelling
When Should Women Start Thinking About Bone Health?
Bone loss doesn’t begin suddenly after menopause; but it may accelerate during transition. Experts recommend that women may benefit by paying attention to bone health10,11:
- During late 30s and 40s
- At the onset of perimenopausal symptoms
- If there is a family history of fractures or osteoporosis
Early awareness may allow women to build stronger reserves before rapid bone loss sets in.
Supporting Bones During Menopause
Support bone health during menopause, may involve a multi-pronged approach, which may include:
- Eat balanced diet that includes calcium rich diet, dairy products
- Ensuring sufficient Calcium and Vitamin D3
- Staying physically active – Resistance, balance and weight bearing exercises
- Avoiding smoking and excessive alcohol
- Maintaining overall nutritional balance
For some women, dietary supplements may form a part of this broader preventive strategy to meet changing nutritional needs.
Menopause is a natural transition, but bone loss doesn’t have to be an inevitable consequence.
Understanding the connection between menopause and bone health helps support women to take proactive steps before problems arise. With the right nutritional support, lifestyle habits, and awareness, bones may be supported well beyond menopause.
Because caring for bones today means protecting independence, mobility, and quality of life for years to come.
REFERENCES
1Strelow B et al., Menopause Decoded: What's Happening and How to Manage It. J Prim Care Community Health. 2024 Jan-Dec;15:21501319241307460. doi: 10.1177/21501319241307460.
2Keen MU, Barnett MJ, Anastasopoulou C. Osteoporosis in Females. [Updated 2025 Jun 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559156/
3Demontiero O, Vidal C, Duque G. Aging and bone loss: new insights for the clinician. Ther Adv Musculoskelet Dis. 2012 Apr;4(2):61-76. doi: 10.1177/1759720X11430858.
4Shanbhogue VV, Brixen K, Hansen S. Age- and Sex-Related Changes in Bone Microarchitecture and Estimated Strength: A Three-Year Prospective Study Using HRpQCT. J Bone Miner Res. 2016 Aug;31(8):1541-9. doi: 10.1002/jbmr.2817. Epub 2016 Mar 15. PMID: 26896351.
5Fan Y et al. Sex- and Age-Specific Prevalence of Osteopenia and Osteoporosis: Sampling Survey. JMIR Public Health Surveill. 2024 Apr 5;10:e48947. doi: 10.2196/48947. PMID: 38578689; PMCID: PMC11031699.
6Väänänen HK, Härkönen PL. Estrogen and bone metabolism. Maturitas. 1996 May;23 Suppl:S65-9.
7Ahlborg HG et al. Bone loss in relation to menopause: a prospective study during 16 years. Bone. 2001 Mar;28(3):327-31. doi: 10.1016/s8756-3282(00)00451-8.
8Lo JC, Burnett-Bowie SA, Finkelstein JS. Bone and the perimenopause. Obstet Gynecol Clin North Am. 2011 Sep;38(3):503-17. doi: 10.1016/j.ogc.2011.07.001. PMID: 21961717; PMCID: PMC3920744.
9Qureshi HJ, Hussain G, Jafary ZA, Bashir MU, Latif N, Riaz Z. Calcium status in premenopausal and postmenopausal women. J Ayub Med Coll Abbottabad. 2010 Apr-Jun;22(2):143-5. PMID: 21702289.
10Stokes G, Herath M, Samad N, Trinh A, Milat F. 'Bone Health-Across a Woman's Lifespan'. Clin Endocrinol (Oxf). 2025 Apr;102(4):389-402. doi: 10.1111/cen.15203.
11McPhee C, Aninye IO, Horan L. Recommendations for Improving Women's Bone Health Throughout the Lifespan. J Womens Health (Larchmt). 2022 Dec;31(12):1671-1676. doi: 10.1089/jwh.2022.0361.
12BONE HEALTH AND POSTMENOPAUSAL WOMEN. AN ENDOCRINE SOCIETY PATIENT RESOURCE